Pediatric Abusive Head Trauma CE for Kentucky Nurses
Prevent and Report Shaken Baby Syndrome
Online Continuing Education Course
Course Description
MANDATORY KENTUCKY NURSING CEU. Fulfills the requirement for 1.5 hours of continuing education on recognizing and preventing PAHT (pediatric abusive head trauma) for nurses. Covers risk factors, assessment and diagnosis, prevention strategies, and KY standards for reporting child abuse and neglect.
Course Price: $20.00
Contact Hours: 1.5
Course updated on
March 18, 2025
"Thank you for providing this opportunity to learn more about PAHT, increase my awareness of this subject, and also for providing the opportunity to meet the KY state board requirement." - Jane, RN in Kentucky
"Great! Loved the format and the ability to see the content and exam. Very informative and thorough." - Mary, RN in Kentucky
"Excellent offering that provided eye-opening education applicable to our society. Valuable learning experience." - Linda, RN in Kentucky
"The information is so WELL defined. One can tell the amount of time and effort that went into developing this course. EXCELLENT JOB!" - Anna, RN in Kentucky
Pediatric Abusive Head Trauma CE for Kentucky Nurses
Prevent and Report Shaken Baby Syndrome
Copyright © 2025 Wild Iris Medical Education, Inc. All Rights Reserved.
LEARNING OUTCOME AND OBJECTIVES: Upon completion of this course, you will be better prepared to recognize and help prevent pediatric abusive head trauma (AHT) and understand reporting requirements for instances of AHT in Kentucky. Specific learning objectives to address potential knowledge gaps include:
- Define pediatric “abusive head trauma” (AHT).
- Recognize the risk factors for head injuries resulting from abuse.
- Describe the mechanisms of injury, clinical presentation, history gathering, physical assessment, and diagnosis of pediatric AHT.
- Distinguish between accidental and abusive head trauma in the pediatric population, including controversies surrounding diagnosis.
- Summarize primary, secondary, and tertiary resources for prevention of pediatric AHT.
- Discuss Kentucky reporting requirements for suspected child abuse and neglect.
TABLE OF CONTENTS
INTRODUCTION
According to the CDC (2024), abusive head trauma (AHT) is a severe form of child abuse that results in a brain injury. It is often caused by violent shaking (referred to as shaken baby syndrome) or blunt impact. The resulting injury can cause bleeding around the brain or behind the eyes. AHT includes a range of injury mechanisms and clinical outcomes, from subtle presentations to infants with severe and life-threatening injuries.
The diagnosis of AHT should be made by a team of specialists from different medical disciplines, who will consider all available evidence, including physical examinations, imaging tests (radiographs), lab results, and the child’s developmental stage, to ensure the findings cannot be explained by a plausible, nonabusive cause. If necessary, further consultation with specialists like radiologists, ophthalmologists, neurosurgeons, neurologists, and pediatric surgeons should be involved to thoroughly evaluate the case and reach an accurate diagnosis (AAP, 2020; Choudhary et al., 2018, O’Meara et al., 2020).
AHT continues to be a leading cause of physical abuse–related death in children and the leading cause of death from injury in infants. Nearly all victims of abusive head trauma suffer serious, long-term health consequences, including vision problems, developmental delays, physical disabilities, and hearing loss. As many as 1 of every 4 babies who experience abusive head trauma dies from this form of child abuse (CDC, 2024). (See also “Risk Factors” below.)
For children in the first year of life, the majority of serious head injuries result from abuse, and this peak incidence and rapid decrease with age are thought to be related to episodes of prolonged, inconsolable, and unpredictable crying. Such crying can be both a developmentally typical way for infants to communicate their basic needs, but it also can be related to a variety of other health or developmental causes that can be identified through medical examination. Regardless of the etiology, it is important to aim prevention strategies toward supporting parents and caregivers in dealing with crying.
TERMINOLOGY
- Pediatric abusive head trauma (PAHT or AHT)
- KRS 620.020 defines pediatric abusive head trauma as the various injuries or conditions that may result following the vigorous shaking, slamming, or impacting the head of an infant or young child. These injuries or conditions, also known as pediatric acquired abusive head trauma, have in the past been called Shaken Baby Syndrome or Shaken Infant Syndrome. Pediatric abusive head trauma injuries or conditions have included but are not limited to the following:
- Irreversible brain damage
- Blindness
- Retinal hemorrhage
- Eye damage
- Cerebral palsy
- Hearing loss
- Spinal cord injury
- Paralysis
- Seizures
- Learning disability
- Death
- Central nervous system injury as evidenced by central nervous system hemorrhaging
- Closed head injury
- Rib fracture
- Subdural hematoma
(KY General Assembly, 2025)
- Pediatric acquired/traumatic brain injury (PA/TBI)
- This term includes traumatic causes such as those sustained as a result of motor vehicle accidents, sports-related injuries, blast injuries from war, assaults or child abuse, gunshot wounds, and falls.
- Shaken baby syndrome (SBS)
- SBS refers to a form of abusive head trauma caused by shaking and with a characteristic pattern of injuries that may include retinal hemorrhages, certain fractures (in particular, ribs and the ends of long bones), and recognizable patterns of brain injury, often including thin subdural hemorrhages and sometimes diffuse axonal injury.
The change in terminology (from shaken baby syndrome to abusive head trauma) was misinterpreted by some in the legal and medical communities as an invalidation of the diagnosis and the mechanism of shaking as a cause of injury. However, the AAP continues to affirm the dangers and harms of shaking infants and embraces the “shaken baby syndrome” diagnosis as a valid subset of an AHT diagnosis and for parental education and community preventative efforts to caution against the detrimental effects of infant shaking (AAP, 2020).
RISK FACTORS FOR ABUSIVE HEAD TRAUMA
Anatomy- and Physiology-Related Risk Factors
There are specifics risks to a young infant due to their anatomy and physiology. These include the combination of a disproportionally larger head, soft and rapidly growing brain, thin skull wall, and lack of mobility and control of the head and neck that makes infants extremely vulnerable to injury from shaking actions.
The anatomic characteristics of a child’s brain render it more susceptible than the adult brain to certain types of injuries following head trauma. The head is larger in proportion to the body surface area, and stability is dependent on the ligamentous rather than bony structures (Verive, 2023). Because the brain grows rapidly during infancy, infants have proportionally larger heads than adults in relation to their body size. (The relation between head and body size continuously declines with increasing age.) Therefore, the head is relatively heavy compared to the rest of the body, which results in different dynamics of head acceleration due to external forces, making the infant head more vulnerable to trauma (Araki et al., 2017).
Additionally, the infant’s brain has higher water content and less myelination than an adult brain, is more gelatinous, and is easily compressed and distorted within the skull during a shaking episode. The infant’s blood vessels around the brain are more susceptible to shearing, and tearing can lead to brain hemorrhages. Because of their minimally developed anatomy, infants are also at increased risk for death and permanent disability.
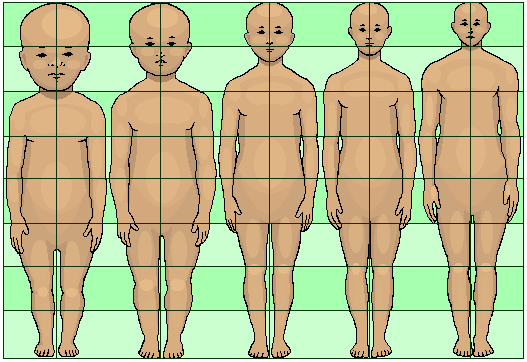
Diagram showing the proportionally larger head of an infant relative to an adult. (Source: Journal of Heredity, 1921.)
Parent / Caregiver Risk Factors
Understanding the risks of AHT from various caregivers may help to inform current prevention strategies. A critical risk factor is the occurrence of shaking used either to attempt to calm infants and children or as a means of discipline. Other risk factors include socioeconomic status, societal and family stress, prematurity, multiple births, developmental delay, and childhood history of abuse in the parent or caregiver.
There are few statistics for risk factors specific to abusive head trauma. Among the limited studies, it is commonly reported that parents were more likely to be perpetrators of the confirmed or suspected child abuse. However, children injured by a parent’s partner—a group that was overwhelmingly male—were more likely to be more severely injured, to experience severe head injuries, and to require intubation compared with children who were abused by a parent.
Laurent-Vannier and colleagues (2021) examined 91 cases of AHT and found that all of the abusive events occurred inside a home (parent’s or childcare provider’s), never outdoors or in a public place, and always in the presence of only one adult. One third of perpetrators were male (n = 32), and two thirds female (n = 59), of which 49 were the childcare provider (“nanny”) and 10 were the infant’s mother. Another study found the percentage of women that shake infants might be higher than previously thought.
Intimate partner violence and adverse childhood experiences (ACEs) are also key risk factors for shaking and harmful parenting behaviors in general (Berthold et al., 2024). These may include traumatic events, such as violence, abuse, or neglect, that occur in childhood and negatively affect a child’s brain development. These disruptions increase the risk of poor physical health, coping skills, or other long-term cognitive impairments (CDC, 2024c).
Risk factors for child abuse in general are described below.
(See also “Protective Factors” later in this course.)
INDIVIDUAL RISK FACTORS IN CAREGIVERS
- Drug or alcohol issues
- Mental health issues, including depression
- Not understanding children’s needs or development
- Abuse or neglect as children
- Being young, single, or having many children
- Low education or income
- Experiencing high levels of parenting stress or economic stress
- Using spanking and other forms of corporal punishment for discipline
- Not being a child’s biological parent
- Holding attitudes accepting of or justifying violence or aggression
(CDC, 2024b)
RELATIONSHIP / FAMILY RISK FACTORS
- Having household members in jail or prison
- Being isolated from and not connected to other people (extended family, friends, neighbors)
- Experiencing other types of violence, including relationship violence
- High levels of conflict
- Negative communication styles
(CDC, 2024b)
COMMUNITY RISK FACTORS
- High rates of violence and crime
- High rates of poverty and limited educational and economic opportunities
- High unemployment rates
- Easy access to drugs and alcohol
- Neighbors who don’t know or look out for each other
- Low community involvement among residents
- Few community activities for young people
- Unstable housing and residents who move frequently
- Frequent food insecurity
(CDC, 2024b)
It is also important to note that there is limited and inconsistent evidence on the validity and reliability of risk assessment instruments in primary care settings. The literature describes that the use of such instruments may cause harm, including social stigmas and effects on family functioning and dynamics, due to inaccuracies in screening questions and ethnic bias (Hart et al., 2024).
Child Risk Factors
Children with disabilities or special healthcare needs—including those born prematurely or having developmental delays or disabilities—are at higher risk for AHT. A lack of understanding of premature infant development may lead to additional frustration, stress, decreased tolerance, and resentment among caregivers. Since premature infants have a higher rate of disabilities than full-term infants, their risk is even greater.
Infants experiencing neonatal abstinence syndrome (NAS) (i.e., babies in withdrawal) are at particular risk for child abuse, including abusive head trauma, due to the irritability and excessive crying that result from withdrawal from substance addiction. This can last for weeks and months, making such babies difficult to care for.
ASSESSMENT AND DIAGNOSIS OF PEDIATRIC ABUSIVE HEAD TRAUMA
Mechanism of Injury
Abusive head trauma encompasses many mechanisms of injury. Children who present with AHT may have been injured due to shaking, blunt impact, suffocation, strangulation, and other causes. It is important to remember that no single injury is diagnostic of AHT (Choudhary et al., 2018).
Each type of imposed stress produces a characteristic pattern of injury:
- Acceleration and deceleration through an arc (shaking) produce thin subdural hemorrhage and, commonly, retinal hemorrhages.
- Impact is associated with skull fractures, contra-coup bruising, and unilateral subdural hemorrhage.
- Strangulation causes hypoxia and hypoxic ischemic encephalopathy.
These stresses may occur separately or in any combination.
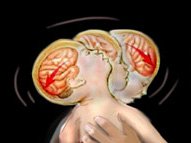
When a baby is shaken, the neck snaps back and forth and the brain rotates, causing shearing stresses on the vessels and membranes between the brain and skull. (Source: Radiologyassistant.nl.)
Clinical Presentations
Healthcare professionals may first encounter young children with AHT in a range of clinical settings, including primary care, urgent care, and emergency departments. Since there are significant variations in the clinical presentation of children with AHT, it is important that professionals are trained to identify potentially life-threatening situations.
While there is an increased awareness about AHT and how it may present, it is still important to realize that AHT may present with subtle signs and symptoms. A history of trauma is rarely reported in the initial assessment stages, and if it is, it is usually reported as a fall from a distance of less than five feet (APA, 2020).
Less severely injured infants and young children may present with symptoms that are quite nonspecific and without a history of trauma provided by a caregiver. These symptoms may be transient and improve if the trauma is not repeated. They include irritability, vomiting, and apnea. These and other symptoms of AHT are also seen in other minor medical conditions and can easily lead to a mistaken diagnosis of those conditions instead. Healthcare providers may have difficulty recognizing that such symptoms are the result of abuse, and the infant may return to an abusive environment (see also “Differential Diagnoses” below).
More seriously injured children have symptoms that should lead to rapid diagnosis of intracranial trauma. The caregiver may report a dramatic change in level of consciousness, as in acute collapse, such as unconsciousness, apnea, or seizures. An episode of minor trauma may be given as an explanation for the injury. Examples include falls off beds, being dropped by caregivers, or other minor contact injuries to the head.
Presenting History
Any reported history or statements made by the caregiver regarding the injury should be documented accurately and completely. It is best to include the specific questions asked as well as the responses. Information should be gathered in a nonaccusatory but detailed manner.
There are two general portions of the presenting history that are important to document. The first is the history of the injury event, and the second is how the child responded or behaved after the injury.
Questions asked when taking a presenting history should include:
- What happened?
- Who was there when it happened?
- Where did it happen?
- When did it happen?
- What happened afterwards?
- When was the child noticed to be ill or injured? How did the child respond? When did symptoms start? How did you respond?
- What made you bring the child to the doctor (or hospital)?
- When was the last time the child was totally normal or well?
- What has the child been doing and how have they appeared during the last 24–48 hours?
Medical, Developmental, and Social History
Information that may be useful in the medical assessment of suspected physical abuse includes:
- Past medical history (trauma, hospitalizations, congenital conditions, chronic illnesses)
- Nutrition history
- Seizure history
- Medications and immunizations
- Family history (especially of bleeding, bone disorders, and metabolic or genetic disorders, which often appear as a history of early deaths)
- Pregnancy history (wanted/unwanted, planned/unplanned, prenatal care, postnatal complications, postpartum depression, delivery in a nonhospital setting)
- Familial patterns of discipline
- Child temperament (easy to care for versus fussy)
- History of past abuse to child, siblings, or parents, including history of CPS or police involvement
- Developmental history of child (language, gross motor, fine motor, psychosocial milestones)
- Substance abuse by any caregivers or people living in the home
- Social and financial stressors and resources (unemployment, divorce/separation, etc.)
- Violent interactions among other family members
(Christian & Levin, 2018)
The social history is a critical component of the evaluation. Asking parents about the household composition, other caregivers, siblings, substance abuse, mental illness, and social stressors can provide valuable information. It is preferable to interview caregivers separately; thorough and accurate documentation, including the use of quotes, is critical.
CAUSES FOR CONCERN
Examples of findings that are of concern for possible AHT include:
- Any infant or young child whose history is not plausible or consistent with the presenting signs and symptoms (i.e., explanation that is inconsistent with the pattern, age, or severity of the injury or injuries)
- History of behavior that is inconsistent with the child’s physical or developmental capabilities
- Presence of a new adult partner in the home
- History of delay in seeking medical attention
- History or suspicion of previous abuse
- Absence of a primary caregiver at the onset of injury or illness
- Physical evidence of multiple injuries at varying stages of healing
- Unexplained changes in neurologic status, unexplained shock, or cardiovascular collapse
Physical Assessment
There are various signs and symptoms of AHT that can be recognized in a physical assessment of the child. Depending on the severity of the clinical presentation, initial assessment is often focused on identifying and treating life-threatening issues. This initial assessment focuses on the airway, breathing, circulation, and neurologic status.
As noted above, the consequences of less severe cases may not be brought to the attention of healthcare professionals and may never be diagnosed. In the most severe cases, which usually result in death or severe neurological consequences, the child usually becomes immediately unconscious and suffers rapidly escalating, life-threatening central nervous system dysfunction.
Common presenting signs and symptoms of AHT are:
- Lethargy/decreased muscle tone
- Extreme irritability
- Decreased appetite, poor feeding, or vomiting for no apparent reason
- Grab-type bruises on arms or chest
- No smiling or vocalization
- Poor sucking or swallowing
- Rigidity or posturing
- Difficulty breathing
- Decreased level of consciousness
- Seizures
- Head or forehead appears larger than usual
- Fontanel (soft-spot) on head appears to be bulging
- Inability to lift head
- Inability of eyes to focus or track movement
- Unequal size of pupils
(NCSBS, n.d.-a)
Complete physical exam for any young child with suspected AHT includes:
- Inspection of all body parts, scalp, ears, and hair
- Inspection of the mouth (lip, tongue, buccal) to observe for frenula tears or dental injuries
- Palpation of legs, arms, hands, feet, and ribs to assess for crepitus or deformities
Nursing neurologic assessment of the child with head trauma includes evaluation of:
- Eye opening
- Arousability level or irritability/consolability
- Symmetry of facial expressions
- Movement of upper and lower extremities
- Increased weakness or pitch in cry/vocalizations
- Fontanels
- Each pupil separately for size, shape, equality of reaction to light
- Ability to track objects
- Muscle tone for rigid extension or flexion of extremities, flaccidity, or unusual posturing
Research has identified several specific types of injuries as being associated with AHT. These include retinal hemorrhage in 85% of cases, subdural hematoma in over 70%, and hypoxic-ischemic injury and cerebral edema as significantly associated with AHT (O’Meara et al., 2020).
CHILD ABUSE PEDIATRIC (CAP) SPECIALISTS
Child Abuse Pediatric (CAP) subspecialists are responsible for evaluating, diagnosing, and treating the pediatric population for suspected child maltreatment. Arriving at a correct diagnosis has significant ramifications for the child and family. In addition to clinical care, CAP subspecialists act as a resource for their communities, providing education and guidance to medical and mental health providers, child protective services (CPS), law enforcement, and community agencies. They also participate in death reviews and provide testimony at court proceedings.
Despite the high rates of child abuse and neglect, CAP is one of the smallest pediatric subspecialties, considering it works with some of the most vulnerable children and families, and engages with a variety of other pediatric stakeholders. The CAP workforce faces numerous challenges, including few fellows entering the field, decreased financial compensation compared with other fields of medicine, and threats to workforce retention, including secondary trauma and harmful exposure in the media (Slingsby et al., 2024).
Distinguishing Between Accidental and Abusive Head Trauma
There are several challenges to differentiating between accidental (nonabusive/noninflicted) trauma or age-appropriate injuries and child abuse in infants and young children. This is especially true in children who are not yet verbal enough to explain what happened to them (i.e., infants, toddlers, and children with developmental delay or altered levels of consciousness).
Because of this, knowledge of typical developmental patterns of injury is helpful. That is, how does the presenting pattern(s) of injury and the child’s age and developmental level match up with the reported mechanism of injury?
DEVELOPMENTAL PATTERNS OF INJURY
Developmental patterns of injury seen in the 0- to 3-year-old range (the age range most frequently seen with AHT) include:
- Trauma from falls from furniture, down stairs, or being dropped by another person
- Traumatic delivery (e.g., forceps, vacuum extraction, or breech)
- Motor vehicle accidents
Head injury is frequently involved with these traumas because of several factors, including the larger head-to-body ratio and the inability to shield oneself during a fall.
Developmentally, this age range is at risk for accidental injury because the child’s developmental milestones include increasing motor skills and curiosity, allowing them a greater range and access to potential hazards. The advancing physical abilities of young children often precede their ability to understand the consequences of their actions. Thus, parent/caregiver knowledge of growth and developmental milestones may reduce the likelihood that they will misjudge the ability of the child and utilize an inappropriate supervision strategy. The mechanisms seen in accidental (noninflicted) injuries are generally different in these types of injuries as compared to AHT, as discussed below.
ASSESSMENT QUESTIONS
Because this situation is highly charged for both the family and all the healthcare providers involved, it is a good idea to have a checklist in place to both pose questions and evaluate responses in relation to the specific patient in question. Providers should objectively and clearly document the history as described by the parents or caregivers present.
The following are questions a clinician can ask themself to help separate the unintentional from the inflicted injury:
- What is the age of the child?
- What are the normal behaviors of a child at that age? Developmental stages of childhood determine what kinds of injuries are likely to be seen. The motor skills of the child determine what the child could have done to incur injury.
- Based on the child’s age, is the presenting injury plausible?
- Is the history plausible? Could this injury have been sustained in the manner described? Does the history change with changing information supplied to the caretaker? Adjustments in the account of the injury may be made by caretakers to fit the evolving information, indicating the tailoring of the history to fit new information. Does the history change when related in subsequent accounts by other family members?
- Was the injury witnessed? The lack of information as to how a serious injury has occurred should raise the index of suspicion for an abusive origin.
- Is the social situation in which the injury occurred a high-risk environment? The presence of community or intrafamilial violence, substance abuse, chaotic living arrangements, poverty, social isolation, transient lifestyles, mental health issues, and conflict among family members are red flags.
- Can the described mechanism of injury account for the observed injury? What else could produce the clinical picture?
- Can the history be independently verified (through photographs, scene investigation, etc.)?
Explanations that are concerning for intentional trauma include:
- No explanation or vague explanation for a significant injury
- An important detail of the explanation that changes dramatically
- An explanation that is inconsistent with the pattern, age, or severity of the injury or injuries
- An explanation that is inconsistent with the child’s physical or developmental capabilities
- Different witnesses who provide markedly different explanations for the injury or injuries
(Christian, 2015)
(See also “Reporting Child Abuse and Neglect” below for information on when a healthcare provider may be mandated to report suspected AHT.)
Differential Diagnoses
It is also important to rule out underlying conditions that may cause some of the same signs or symptoms associated with AHT or other abuse. Where indicated, medical professionals should inquire about the presence of any of the following conditions or practices:
- Congenital, metabolic, or neoplastic conditions (e.g., aneurysm, arteriovenous malformation, brain tumor, leukemia)
- Connective tissue disease or osteogenesis imperfecta, which may lead to fragile bones that fracture with less force than would be expected
- Acquired causes (e.g., meningitis, obstructive hydrocephalus)
- Undetected bleeding disorders that can lead to abnormal bleeding patterns (e.g., hemophilia, Von Willebrand’s disease, liver disease)
- Traditional or alternative healing practices, which may lead to unusual bruising and scarring patterns (e.g., coin rubbing, cupping, or burning herbs on the skin over acupuncture points)
(Waters-Tozier, 2020)
MEDICOLEGAL CONTROVERSIES SURROUNDING POTENTIAL MISDIAGNOSIS OF ABUSIVE HEAD TRAUMA
There has been significant medicolegal media attention related to the potential misdiagnosis of AHT (Colloff, 2024; Lennon, 2024). It is important that healthcare providers are aware of these controversies and keep current on the challenges of diagnosing AHT.
Because AHT is considered by some to be a commonly misdiagnosed condition, several systematic reviews have looked at the compiled research on diagnosis. Maiese and colleagues (2021) evaluated the current scientific evidence on best practices, including the importance of circumstantial evidence, clinical history, the use of postmortem radiological examinations (such as CT and MRI), and autopsy.
Tibballs and Bhatia (2024) reviewed AHT cases from Australia, the United Kingdom, and the United States. They reported “that on expert opinion alone, a ‘triad’ of clinical signs (severe retinal hemorrhages, subdural hematoma, and encephalopathy) is dogmatically attributed diagnostically to severe deliberate shaking with or without head trauma. However, the evidence for this mechanism is of the lowest scientific level and of low to very-low quality and therefore unreliable. Consequently, expert opinion should not determine legal outcomes in prosecuted cases. Expert witnesses should reveal the basis of their opinions and the uncertainties and controversies of the diagnosis.” This review suggested abandonment of the inherently inculpatory diagnostic terms shaken baby syndrome and abusive head trauma and their appropriate replacement with infantile retinodural hemorrhage.
An earlier review by Lindberg and colleagues (2019) reported that new science is changing accepted medical opinion about abusive head injury that has frequently made the medicolegal press involving abusive head trauma. The review analyzed published scientific articles about AHT to determine whether this new information has led to significant changes in the understanding, evaluation, and management of children with suspected AHT. They concluded that:
- The overwhelming weight of recent data does not change the fundamental consensus.
- Abusive head trauma is a significant source of morbidity and mortality in children.
- Subdural hematomas and severe retinal hemorrhages are commonly the result of severe trauma.
- These injuries should prompt an evaluation for abuse when identified in young children without a history of such severe trauma.
- Short falls, cerebral sinus thrombosis, and vaccinations are not plausible explanations for findings that raise concern for abusive head trauma.
PREVENTION STRATEGIES FOR ABUSIVE HEAD TRAUMA
There is an increasing focus on ways that healthcare providers have a unique opportunity to support families in forming and maintaining relational health, defined as safe and stable relationships that protect and nurture a child’s growth and development, thereby helping to prevent child abuse (Stirling et al., 2024).
Protective Factors
Research has shown that certain protective factors are linked to a lower incidence of child abuse and neglect in general. They are attributes that serve as buffers, helping parents who might otherwise be at risk of abusing their children to find resources, supports, or coping strategies that allow them to parent effectively, even under stress.
Individual protective factors in caregivers include:
- Creating safe, positive relationships with children
- Practicing nurturing parenting skills and providing emotional support
- Meeting basic needs of food, shelter, education, and health services
- Having a college degree or higher and having steady employment
Relationship/family protective factors include:
- Having strong social support networks and stable, positive relationships
- Being present and interested in the child
- Enforcing household rules and engaging in child monitoring
- Having caring adults outside the family who can serve as role models or mentors
Community protective factors include:
- Access to safe, stable housing
- Access to high-quality preschool
- Access to nurturing and safe childcare
- Access to safe, engaging afterschool programs and activities
- Access to medical care and mental health services
- Access to economic and financial help
- Access to work opportunities with family-friendly policies
CDC (2024b)
Alternative approaches are now being considered that support the above protective factors. These include:
- Creating and validating a broader array of family well-being outcomes that are correlated with child well-being (e.g., parental stress, access to resources)
- Expanding research on the drivers of, interventions for, and consequences of racial and ethnic bias in addressing child maltreatment
- Increasing study of risk factors that include adversity faced by families in the form of access to childcare, healthcare (particularly mental health and substance use treatment), housing, and food insecurity
- Considering population-level metrics for measurement of child maltreatment
- Increasing study of policy-level changes to improve the well-being of children, such as tax credits, expanded subsidies for childcare, and guaranteed paid parental leave
(Hart et al., 2024)
For example, research on state paid family leave (PFL) policies as a community/societal protective factor suggest that PFL has a beneficial effect on infant maltreatment rates and adds to the growing evidence that policies aimed to support household economic stability could be a vital child maltreatment prevention policy tool (Tanis et al., 2024).
SOCIAL-ECOLOGICAL MODEL
Social-ecological theory examines how people exist within and are shaped by their individual characteristics, families and other relationships, communities, and society. The overlapping rings of the graphic below illustrate how protective factors against potential child abuse at one level influence factors at other levels.
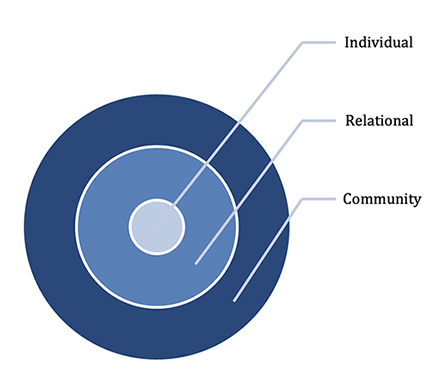
Community/society protective factors
- Community norms of shared responsibility for supporting parents and families
- Implementation of evidence-based practices
- Access to basic needs and specialized services
Relational protective factors
- Relationships with peers and reduced feelings of isolation
- Positive relationships within the extended family
- Ability to communicate emotions effectively
- Engagement in social institutions (e.g., schools, faith communities)
- Secure parent–child relationships
Individual protective factors
- Stress management
- Access to concrete support
- Hopefulness
- Problem-solving skills
- Resilience
- Parenting skills
(CWIG, 2020)
Prevention Continuum to Strengthen Families
Prevention and child welfare policies can be viewed across a spectrum of comprehensive supports. Primary prevention efforts address a broad segment of the population, such as all new parents. Secondary prevention efforts target a specific subset of the population considered to be at higher risk for child maltreatment. Tertiary prevention efforts target perpetrators of child maltreatment and seek primarily to prevent recidivism (CWIG, n.d.).
PRIMARY EFFORTS: GENERAL POPULATION AND PARENT EDUCATION
Many states, including Kentucky, have enacted programs aimed at preventing child abuse, including pediatric abusive head trauma, through a public health primary universal prevention strategy aimed at changing knowledge and behaviors of caregivers and society in general concerning normal development of infants and the significance of early increased infant crying. By increasing parental understanding of infant development, with a focus on infant crying and coping strategies to address it, such programs are thought to offer a “window of opportunity” for the prevention of AHT and, potentially, other forms of infant abuse.
Primary prevention activities are directed at the general population and attempt to stop maltreatment before it occurs. All members of the community have access to and may benefit from these services. Primary prevention activities with a universal focus seek to raise the awareness of the general public, service providers, and decision makers about the scope and problems associated with child maltreatment.
Healthcare professionals can provide the following messages to parents and caregivers during their everyday encounters:
- Remind parents and caregivers that crying is normal for babies.
- Explain to parents that excessive crying is often a normal phase of infant development.
- Ask parents how they are coping with parenthood and their feelings of stress.
- Assure parents that it is normal to feel frustrated at long bouts of crying and a sudden decrease in sleep but that things will get better.
- Give parents the number to a local helpline or other resource for help.
- Talk with parents about the steps they can take when feeling frustrated with a crying baby, such as putting the baby safely in a crib on their back, checking on the baby’s safety every 5 to 10 minutes, and calling for help or a friend.
- Let parents know what to check for when their baby is crying: signs of illness, fever, or other behavior that is unusual; discomfort like a dirty diaper, diaper rash, teething, or tight clothing; or whether the baby is hungry or needs to be burped.
(CBCS, 2021)
Period of PURPLE Crying
The Period of PURPLE Crying is an example of a primary-level program specifically geared to the prevention of AHT. The target population is all parents of new infants and society in general, with the goal of increasing their understanding of early infant crying and shaken baby syndrome. The Period of Purple Crying training, when taken by nurses, has also been shown to improve nurses’ short- and long-term understanding of AHT and their confidence in instructing parents and caregivers about its associated dangers and risks (Dias et al., 2021).
| (NCSBS, n.d.-b) | ||
| P | Peak of crying | Your baby may cry more each week, peaking at 2 months, then less at 3 to 5 months. |
| U | Unexpected | Crying can come and go, and you do not know why. |
| R | Resists soothing | Your baby may not stop crying no matter what you try. |
| P | Pain-like face | Your crying baby may look to be in pain even when they are not. |
| L | Long lasting | Crying can last as much as 5 hours a day or more. |
| E | Evening | Your baby may cry more in the late afternoon or evening. |
The PURPLE program includes a booklet plus either a smart phone “app” that parents can use to track crying and access other developmental and anticipatory guidance information or a DVD. The program is designed to help parents of new babies, caregivers, and the public to understand the typical crying curve and the dangers of reacting to an infant’s crying in frustration and shaking a baby. It is based on over 30 years of scientific research on the connection between the infant crying curve and the incidence of SBS and is delivered using a specific protocol (NCSBS, n.d.-b).
(See also “Resources” at the end of this course.)
SECONDARY PREVENTION EFFORTS
Secondary prevention efforts, such as home visitation programs, target a specific subset of the population considered to be at higher risk for child maltreatment due to factors such as poverty, parental substance abuse, young maternal age, parental mental health concerns, and parental or child disabilities. Approaches to prevention programs that focus on high-risk populations might include:
- Parent education programs located in high schools and focusing on teen parents or located within substance abuse treatment programs for mothers and families with young children
- Parent support groups that help parents deal with their everyday stresses and meet the challenges and responsibilities of parenting
- Respite care for families who have children with disabilities or special healthcare needs
- Family resource centers that offer information and referral services to families living in low-income neighborhoods
- Home visiting programs that provide support and assistance to expecting and new mothers in their homes
(CWIG, n.d.)
Nurse-Family Partnership
The Nurse-Family Partnership program provides home visits by registered nurses to first-time, low-income mothers, beginning during pregnancy and continuing through the child’s second birthday. It operates nationwide. The program has three primary goals: 1) to improve pregnancy outcomes by promoting health-related behaviors; 2) to improve child health, development, and safety by promoting competent caregiving; and 3) to enhance parent life-course development by promoting pregnancy planning, educational achievement, and employment. The program also has two secondary goals: 1) to enhance families’ material support by providing links with needed health and social services and 2) to promote supportive relationships among family and friends (NFP, 2023).
Health Access Nurturing Development Services (HANDS)
Kentucky’s HANDS program is an example of a program designed to assist overburdened first-time parents at critical development points. Frequent pre- and postnatal home visits by trained professionals are provided to first-time parents. These appointments assist new parents by sharing important information, problem solving, and helping them to meet basic needs such as housing, food, healthcare, and other required services. All of Kentucky’s 120 counties offer the HANDS program at no cost to families. Enrollment must be during pregnancy or when the infant is less than 3 months old, and referral to HANDS is made through the county health department (KY CHFS, 2025).
TERTIARY PREVENTION EFFORTS
Tertiary prevention activities focus on families where maltreatment has already occurred and seek to reduce the negative consequences of the maltreatment and to prevent recidivism. These prevention programs may include services such as:
- Intensive family preservation services with trained mental health counselors that are available to families 24 hours per day for a short period of time (e.g., six to eight weeks)
- Parent mentor programs with stable, nonabusive families acting as role models and providing support to families in crisis
- Parent support groups that help parents transform negative practices and beliefs into positive parenting behaviors and attitudes
- Mental health services for children and families affected by maltreatment to improve family communication and functioning
(CBCS, 2021)
REPORTING CHILD ABUSE AND NEGLECT IN KENTUCKY
Pediatric abusive head trauma is a form of child abuse, and all fifty states, including Kentucky, have statutes that mandate reporting of suspected child abuse and neglect for certain professionals. Familiarity with Kentucky laws will ensure that providers report to the appropriate agency within the required time frame.
Definitions of Child Abuse and Neglect
(From Kentucky Rev. Stat. §600.020)
“Abused or neglected child” means a child whose health or welfare is harmed or threatened with harm when his or her parent, guardian, or other person exercising custodial control or supervision:
- Inflicts or allows to be inflicted upon the child physical or emotional injury as defined in this section by other than accidental means
- Creates or allows to be created a risk of physical or emotional injury as defined in this section to the child by other than accidental means
- Engages in a pattern of conduct that renders the parent incapable of caring for the immediate and ongoing needs of the child, including but not limited to parental incapacity due to a substance use disorder as defined in KRS 222.005
- Continuously or repeatedly fails or refuses to provide essential parental care and protection for the child, considering the age of the child
- Commits or allows to be committed an act of sexual abuse, sexual exploitation, or prostitution upon the child
- Creates or allows to be created a risk that an act of sexual abuse, sexual exploitation, or prostitution will be committed upon the child
- Abandons or exploits the child
- Does not provide the child with adequate care, supervision, food, clothing, shelter, and education or medical care necessary for the child's well-being when financially able to do so or offered financial or other means to do so. A parent or other person exercising custodial control or supervision of the child legitimately practicing the person's religious beliefs shall not be considered a negligent parent solely because of failure to provide specified medical treatment for a child for that reason alone. This exception shall not preclude a court from ordering necessary medical services for a child
- Fails to make sufficient progress toward identified goals as set forth in the court-approved case plan to allow for the safe return of the child to the parent that results in the child remaining committed to the cabinet and remaining in foster care for fifteen (15) cumulative months out of forty-eight (48) months
- Commits or allows female genital mutilation as defined in KRS 508.125 to be committed
“Physical injury” means substantial physical pain or any impairment of physical condition.
“Serious physical injury” means physical injury that creates a substantial risk of death or causes serious and prolonged disfigurement, prolonged impairment of health, or prolonged loss or impairment of the function of any bodily member or organ.
Persons responsible for the child include:
- A “parent” who is the biological or adoptive mother or father of a child
- A person exercising custodial control or supervision or an agency that has assumed the role and responsibility of a parent or guardian for the child but does not necessarily have legal custody of the child
Exception: A parent or other person exercising custodial control or supervision of the child who is legitimately practicing his or her religious beliefs shall not be considered a negligent parent because of failure to provide specified medical treatment for a child for that reason alone. This exception shall not preclude a court from ordering necessary medical services for a child.
Standards for Reporting
(From Kentucky Rev. Stat. §620.030 and §620.050)
Any person who knows or has reasonable cause to believe that a child is dependent, neglected, or abused shall immediately cause an oral or written report, including but not limited to electronic submissions, to be made to a local law enforcement agency or to the Department of Kentucky State Police, the cabinet or its designated representative, the Commonwealth's attorney, or the county attorney by telephone or otherwise.
All persons are required to report, including but not limited to a physician, osteopathic physician, nurse, teacher, school personnel, social worker, coroner, medical examiner, child-caring personnel, resident, intern, chiropractor, dentist, optometrist, emergency medical technician, paramedic, health professional, mental health professional, peace officer, or any organization or agency for any of the above.
Neither the husband–wife nor any professional client–patient privilege, except the attorney–client and clergy–penitent privilege, shall be a ground for refusing to report.
The reporter is not specifically required by statute to provide his or her name in the report. The identity of the reporter shall not be disclosed except:
- To law enforcement officials, the agency investigating the report, or to a multidisciplinary team
- Under court order, after a court has found reason to believe the reporter knowingly made a false report
Making a Report
Reports of pediatric abusive head trauma can be made by calling toll-free:
- Kentucky Child Protection Hotline: 877-KYSAFE1 (877-597-2331)
Before reporting, explain to the child’s caregiver(s) that:
- The child sustained a serious brain injury not explained by the history
- You are a mandated reporter who is legally required to make a child abuse report
- You will contact social services and law enforcement agencies, which will investigate
As stated above, having a social worker present may be helpful.
Avoid sharing details of clinical findings or suggesting possible explanations for the injuries. Such discussions could affect later forensic interviews and child abuse investigations.
Mandated reporting to county child welfare services and law enforcement agencies is required as soon as the reporter has a reasonable suspicion that abuse has occurred. It is not necessary to wait until all assessments are complete. Although there is usually a cross-reporting mandate between child welfare and law enforcement officials, it might not happen immediately. Generally, once law enforcement officials are notified, they will launch an investigation parallel to the child welfare agency’s investigation.
REDUCING IMPLICIT BIAS IN REPORTING
Research shows that bias can contribute to a lower threshold to suspect child abuse in Black children and adolescents and a higher threshold for White children and adolescents (Jackson, 2024). Therefore, it is important for professionals to be aware of the potential for implicit biases and to ensure that such biases do not impact their decision-making. Instead, decisions must be made based on the objective facts of a situation.
A proven strategy to reduce bias and increase awareness regarding one’s own beliefs is to ask oneself the question, would I make a different decision about reporting if the child or family in a situation of suspected child maltreatment or abuse were of a different:
- Race?
- Ethnicity?
- Gender?
- Gender identity?
- Sexual orientation or expression?
- Religion?
- Immigration status?
- Primary spoken language?
- Culture?
- Age?
- Neighborhood where they reside?
- Presence of a disability?
- Occupation?
- Socioeconomic status of the family?
If the answer is yes, bias may be impacting one’s decision to make a report.
Another strategy when assessing information received about a child and their family is to ask analytical and evaluative questions and use critical thinking. This includes:
- Identifying the specific concerns about the current situation
- Gathering adequate information about the current situation
- Analyzing that information to separate facts from assumptions
- Recognizing the possibility of bias in one’s personal opinions
- Developing multiple hypotheses that could explain the situation
- Determining whether making a report is legally required
- If not, determining whether an alternative option is better, such as connecting the individual or family to appropriate services in their community
(NYS OCFS, 2022)
CONCLUSION
Child abuse and neglect remains a serious problem in Kentucky. Pediatric abusive head trauma is one of the most serious types of such abuse and the leading cause of death from injury in infants.
It is important for all healthcare professionals to be aware of the risk factors and signs and symptoms of AHT in the patients they care for, since a diagnosis depends on input from a multidisciplinary team. Kentucky offers a 24-hour hotline number to make a report of abuse or neglect, and any person suspecting child abuse is required to report it immediately.
Various resources are also available to help prevent the behaviors that lead to AHT, including Kentucky’s statewide HANDS program. Prevention education by healthcare professionals serves the important goal of reducing child abuse and neglect, including abusive head trauma.
RESOURCES
Child Welfare Information Gateway
Kentucky Child Abuse/Neglect hotline
877-KYSAFE1 (877-597-2331) (nights/weekends)
Kentucky Child Protection Branch
National Center on Shaken Baby Syndrome
Prevent Child Abuse Kentucky
800-CHILDREN (statewide helpline)
Responding to Child Maltreatment: A Clinical Handbook for Health Professionals (World Health Organization)
REFERENCES
NOTE: Complete URLs for references retrieved from online sources are provided in the PDF of this course.
American Academy of Pediatrics (AAP). (2020). Policy statement: Abusive head trauma in infants and children. https://publications.aap.org
Araki T, Yokota H, & Morita A. (2017). Pediatric traumatic brain injury: Characteristic features, diagnosis, and management. Neurol Med Chir (Tokyo), 57(2), 82–93.
Berthold O, Fegert JM, Brähler E, Jud A, & Clemens V. (2024). Abusive head trauma: The body of the iceberg—A population-based survey on prevalence and perpetrators. Child Abuse & Neglect, 149, Article 106660. https://doi.org/10.1016/j.chiabu.2024.106660
Capacity Building Center for States (CBCS). (2021). Working across the prevention continuum to strengthen families. Children’s Bureau, Administration for Children and Families, U.S. Department of Health and Human Services. https://capacity.childwelfare.gov
Centers for Disease Control and Prevention (CDC). (2024a). About abusive head trauma. https://www.cdc.gov
Centers for Disease Control and Prevention (CDC). (2024b). Risk and protective factors. https://www.cdc.gov
Centers for Disease Control and Prevention (CDC). (2024c). Adverse childhood experiences. https://www.cdc.gov
Child Welfare Information Gateway (CWIG). (2020). Protective factors approaches in child welfare. U.S. Department of Health and Human Services, Administration for Children and Families, Children’s Bureau. https://www.childwelfare.gov
Child Welfare Information Gateway (CWIG). (n.d.). Prevention continuum. https://www.childwelfare.gov
Choudhary AK, Servaes S, Slovis TL, Palusci VJ, Hedlund GL, Narang SK, Moreno JA, et al. (2018). Consensus statement on abusive head trauma in infants and young children. Pediatric Radiology, 48(8), 1048–65. https://doi.org/10.1007/s00247-018-4149-1
Christian CW. (2015). The evaluation of suspected child physical abuse. Pediatrics, 135(5), e1337–54. https://pubmed.ncbi.nlm.nih.gov
Christian CW & Levin AV. (2018). American Academy of Pediatrics clinical report: The eye examination in the evaluation of child abuse. Pediatrics, 142(2), Article e20181411. https://doi.org/10.1542/peds.2018-1411
Colloff P. (2024, December 29). He dialed 911 to save his baby. Then his children were taken away. New York Times. https://www.nytimes.com
Dias MS, Cappos KM, Rottmund CM, Reed ME, Smith KM, deGuehery KA, & Wang M. (2021). Preventing abusive head trauma: Can educating parents reduce the incidence? Pediatric radiology, 51(6), 1093–6. https://doi.org/10.1007/s00247-020-04819-6
Hart LC, Viswanathan M, & Nicholson WK. (2024). Evidence from the USPSTF and new approaches to evaluate interventions to prevent child maltreatment. JAMA Network Open, 7(7), Article e2420591. https://jamanetwork.com
Jackson AM. (2024). Unmasking racial and ethnic disparities in child physical abuse identification. JAMA Netw Open, 7(12), Article e2451546. https://doi.org/10.1001/jamanetworkopen.2024.51546
Kentucky Cabinet for Health and Family Services (KY CHFS). (2025). Health Access Nurturing Development Services (HANDS). https://www.chfs.ky.gov
Kentucky (KY) General Assembly. (2025). Kentucky revised statutes: KRS chapter 20. https://apps.legislature.ky.gov
Laurent-Vannier A, Bernard JY, & Chevignard M. (2021). Abusive head trauma through shaking: Examination of the perpetrators according to dating of the traumatic event. Child Abuse Rev, 30, 283–99. https://onlinelibrary.wiley.com
Lennon JJ. (2024, May 2). The horrible truth about shaken baby syndrome cases. Slate. https://slate.com
Maiese A, Iannaccone F, Scatena A, Del Fante Z, Oliva A, Frati P, & Fineshci V. (2021). Pediatric abusive head trauma: A systematic review. Diagnostics (Basel), 11(4), 734. https://pubmed.ncbi.nlm.nih.gov
National Center on Shaken Baby Syndrome (NCSBS). (n.d.-a). Learn more. https://www.dontshake.org
National Center on Shaken Baby Syndrome (NCSBS). (n.d.-b). Period of PURPLE crying. https://www.dontshake.org
New York State Office of Children and Family Services (NYS OCFS). (2022). 2022 NYS mandated reporter training syllabus.
Nurse-Family Partnership (NFP). (2023). Nurse-Family Partnership overview. https://www.nursefamilypartnership.org
O’Meara A, Sequeira J, & Ferguson N. (2020). Advances and future directions of diagnosis and management of pediatric abusive head trauma: A review of the literature. Frontiers in Neurology, 11. https://www.frontiersin.org
Slingsby B, Bachim A, Leslie LK, & Moffatt ME. (2024). Child health needs and the child abuse pediatric workforce. Pediatrics, 153(Supplement 2), Article e2023063678F. https://doi.org/10.1542/peds.2023-063678F
Stirling J, Gavril A, Brennan B, Sege RD, Dubowitz H, American Academy of Pediatrics, Council on Child Abuse and Neglect. (2024). The pediatrician’s role in preventing child maltreatment: Clinical report. Pediatrics, 154(2), Article e2024067608. https://publications.aap.org
Tanis JM, Klein SM, & Boyke H. (2024). State paid family leave policies and infant maltreatment. Child Abuse & Neglect, 152, Article 106758. https://pubmed.ncbi.nlm.nih.gov
Tibballs J & Bhatia N. (2024). Medical and legal uncertainties and controversies in “shaken baby syndrome” or infant “abusive head trauma.” J Law Med, 31(1), 151–84. https://pubmed.ncbi.nlm.nih.gov
Verive M. (2023). Pediatric head trauma practice essentials. Medscape. https://emedicine.medscape.com
Waters-Tozier S. (2020). Cultural practices and values that can masquerade as child abuse: A literature review and recommendations for the forensic psychologist. Journal of Forensic Psychology, 5(2). https://www.walshmedicalmedia.com







Customer Rating
4.9 / 191 ratings