August 2022
By Anja Grimes
As per the CDC, monkeypox is a rare disease caused by infection with the monkeypox virus. The monkeypox virus is part of the same family of viruses as the variola virus, which causes smallpox. Monkeypox symptoms are similar to smallpox symptoms but milder, and monkeypox is rarely fatal. Monkeypox is not related to chickenpox.
Monkeypox continues to spread across the globe, with cases jumping by 20% over the beginning of August 2022, according to the World Health Organization.
Infections increased by nearly 7,500 to more than 35,000 cases total across 92 countries, but nearly all reported cases are in Europe and the Americas, according to WHO data. Twelve deaths have been reported so far.
How Can Monkeypox Be Identified?
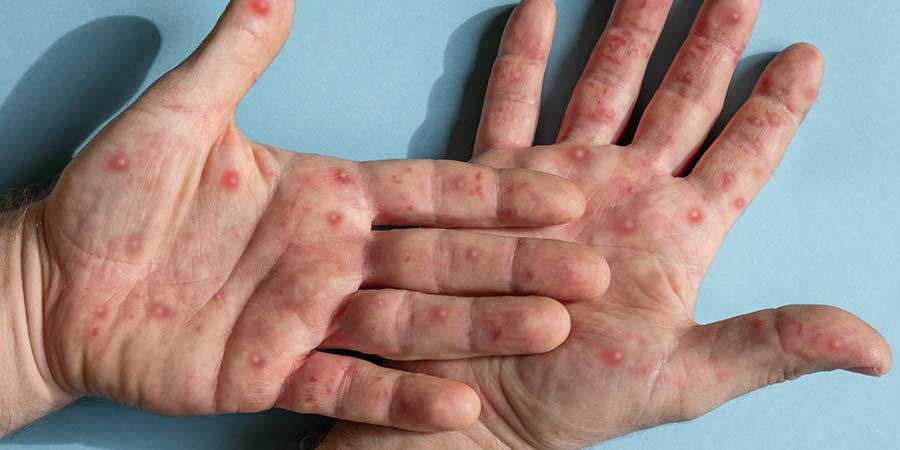
- Lesions are firm or rubbery, well-circumscribed, deep-seated, and often develop umbilication (resembles a dot on the top of the lesion).
- During the current global outbreak:
- Lesions often occur in the genital and anorectal areas or in the mouth.
- Rash is not always disseminated across many sites on the body.
- Rash may be confined to only a few lesions or only a single lesion.
- Rash does not always appear on palms and soles.
- Rectal symptoms (e.g., purulent or bloody stools, rectal pain, or rectal bleeding) have been frequently reported in the current outbreak.
- Lesions are often described as painful until the healing phase, when they become itchy (crusts).
- Lesions typically develop simultaneously and evolve together on any given part of the body. The evolution of lesions progresses through four stages—macular, papular, vesicular, pustular—before scabbing over and desquaming.
The incubation period is 3–17 days. During this time, a person does not have symptoms and may feel fine. The illness typically lasts 2–4 weeks.
The severity of illness can depend upon the initial health of the individual and the route of exposure. The West African virus genetic group, or clade, which is the clade involved in the current outbreak, is associated with milder disease and fewer deaths than the Congo Basin virus clade.
What Are Other Monkeypox Symptoms?

- Fever and other prodromal symptoms (e.g., chills, lymphadenopathy, malaise, myalgias, or headache) can occur before rash but may occur after rash or not be present at all .
- Respiratory symptoms (e.g. sore throat, nasal congestion, or cough) can occur.
How Is Monkeypox Spread/Transmitted?
Monkeypox is not easily transmitted and is not considered a sexually transmitted infection or disease (STI/STD). Transmission via respiratory secretions appears uncommon. Patients generally describe having had close, sustained physical contact with other people with the virus:
Close Contact
Monkeypox can spread to anyone through close, personal, often skin-to-skin contact, including:
- Direct contact with monkeypox rash, scabs, or body fluids from a person with monkeypox
- Touching objects, fabrics (clothing, bedding, or towels), and surfaces that have been used by someone with monkeypox
- Contact with respiratory secretions
Intimate Contact
Direct contact can happen during intimate contact, including:
- Oral, anal, and vaginal sex or touching the genitals or anus of a person with monkeypox
- Hugging, massage, and kissing
- Prolonged face-to-face contact
- Touching fabrics and objects during sex that were used by a person with monkeypox and that have not been disinfected, such as bedding, towels, fetish gear, and sex toys
Monkeypox and Pregnancy
A pregnant person can spread the virus to their fetus through the placenta.
Infected Animals
It’s also possible for people to become infected with monkeypox from infected animals, either by being scratched or bitten by the animal or by preparing or eating meat or using products from an infected animal.
A person with monkeypox can spread it to others from the time symptoms start until the rash has fully healed and a fresh layer of skin has formed. The illness typically lasts 2–4 weeks.
Is There a Treatment for Monkeypox?
There are no treatments specifically for monkeypox virus infections. However, monkeypox and smallpox viruses are genetically similar, which means that antiviral drugs and vaccines developed to protect against smallpox may be used to prevent and treat monkeypox virus infections.
Precautions for Preventing Monkeypox Virus Transmission
In addition to Standard Precautions, if a patient seeking care is suspected to have monkeypox infection, additional infection control precautions (as described below) should be implemented. Infection prevention and control personnel should be notified immediately.
Activities that could resuspend dried material from lesions (e.g., use of portable fans, dry dusting, sweeping, vacuuming) should be avoided.
Patient Placement
A patient with suspected or confirmed monkeypox infection should be placed in a single-person room; special air handling is not required. The door should be kept closed (if safe to do so). The patient should have a dedicated bathroom. Transport and movement of the patient outside of the room should be limited to medically essential purposes. If the patient is transported outside of their room, they should use well-fitting source control (e.g., medical mask) and have any exposed skin lesions covered with a sheet or gown.
Intubation, extubation, and any procedures likely to spread oral secretions should be performed in an airborne infection isolation room.
Personal Protective Equipment (PPE)
PPE used by healthcare personnel who enter the patient’s room should include:
- Gown
- Gloves
- Eye protection (i.e., goggles or a face shield that covers the front and sides of the face)
- NIOSH-approved particulate respirator equipped with N95 filters or higher
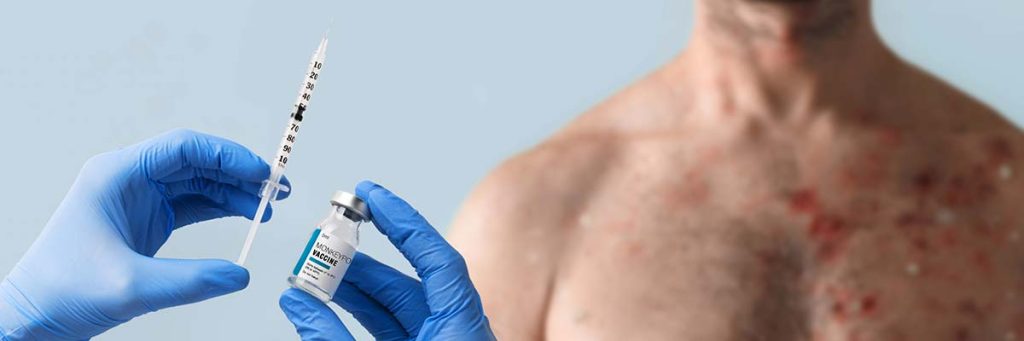
Monkeypox Vaccine Recommendations
CDC recommends vaccination for people who have been exposed to monkeypox and people who may be more likely to get monkeypox.
CDC Print Resources
https://www.cdc.gov/poxvirus/monkeypox/pdf/MonkeyPox-SaferSex-InfoSheet-508.pdf
https://www.cdc.gov/poxvirus/monkeypox/pdf/MPOX-info-teens-young-adults.pdf
Source:
https://www.cdc.gov/poxvirus/monkeypox/index.htm
https://www.cdc.gov/poxvirus/monkeypox/clinicians/clinical-recognition.html
https://www.cdc.gov/poxvirus/monkeypox/symptoms.html
https://www.cdc.gov/poxvirus/monkeypox/vaccines.html
https://www.who.int/health-topics/monkeypox#tab=tab_1
Sign up for our newsletter email list and like us on Facebook and Instagram to be among the first to know about all our special discounts and offers!
About Wild Iris Medical Education:
Wild Iris Medical Education, Inc., is a privately held, woman-owned company providing online healthcare continuing education. In 1998, we began offering online ANCC-accredited nursing continuing education courses and since then have expanded to provide CEUs for occupational therapists, physical therapists, paramedics, EMTs, and other healthcare professionals.
Accredited and Approved Nationwide.
High-quality CEU Courses since 1998.

Join Our More Than 750,000 Satisfied Customers Now!
High-quality, accredited, evidenced-based continuing education courses in an easy-to-use format designed for learning, from Wild Iris Medical Education. We’ve been providing online CE since 1998.